Isha Netralaya | Best Eye Hospital in Mumbai & Pune | Eye Specialist
Hypertensive Retinopathy
What Is Hypertensive Retinopathy?
Hypertensive retinopathy is an eye condition caused by long-standing high blood pressure (hypertension).
When blood pressure remains high for a long time, it damages the small blood vessels of the retina, the light-sensitive layer at the back of the eye responsible for vision.
High blood pressure causes these retinal blood vessels to narrow, leak, or bleed, which can gradually affect eyesight and, in severe cases, lead to permanent vision loss.
Hypertensive retinopathy often develops slowly and silently, especially when blood pressure is not well controlled.
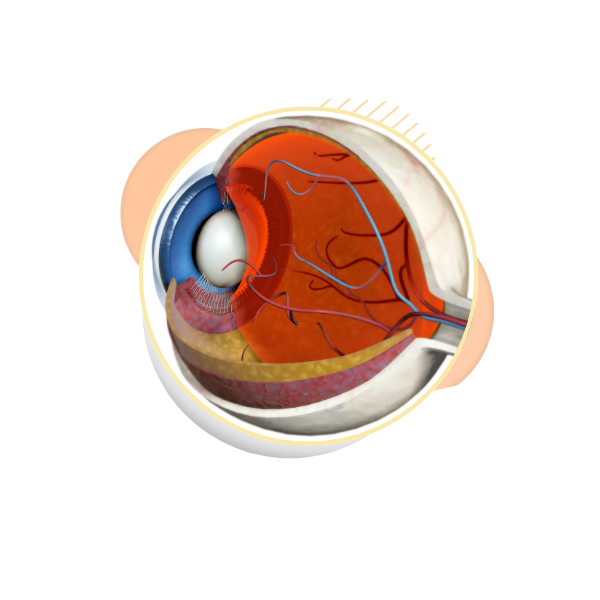
» How High Blood Pressure Affects the Eyes
The retina needs a healthy blood supply to function properly.
When blood pressure is high:
Retinal blood vessels become narrow and stiff
Blood flow to the retina reduces
Fluid or blood may leak into retinal tissue
The optic nerve may swell in severe cases
Over time, this damages the retina’s ability to send clear visual signals to the brain.
» Types of Hypertensive Retinopathy
‣ Mild Hypertensive Retinopathy
Early narrowing of retinal blood vessels
Usually no noticeable symptoms
Detected during routine eye examination
‣ Moderate Hypertensive Retinopathy
More severe vessel narrowing
Leakage of fluid or small bleeding spots
May cause blurred vision
‣ Severe (Malignant) Hypertensive Retinopathy
Significant bleeding in the retina
Swelling of the optic nerve (papilledema)
High risk of serious vision loss or blindness
Medical emergency requiring urgent blood pressure control
» Common Symptoms
Many patients have no symptoms in early stages. As the condition progresses, symptoms may include:
Blurred or distorted vision
Difficulty seeing clearly
Headaches associated with high BP
Seeing spots or floaters
Double vision
Sudden loss of vision (in advanced cases)
⚠️ Vision loss can occur without warning, which is why regular eye check-ups are important.
» Who Is at Higher Risk?
You are at increased risk if you have:
Long-term or poorly controlled high blood pressure
Diabetes
High cholesterol
Kidney disease
Smoking or tobacco habit
Pregnancy with hypertension
The longer blood pressure remains uncontrolled, the higher the risk of retinal damage.
» Who Is at Higher Risk?
You are at increased risk if you have:
Long-term or poorly controlled high blood pressure
Diabetes
High cholesterol
Kidney disease
Smoking or tobacco habit
Pregnancy with hypertension
The longer blood pressure remains uncontrolled, the higher the risk of retinal damage.
» Diagnosis
Hypertensive retinopathy is diagnosed through a detailed dilated eye examination, which allows the doctor to examine retinal blood vessels.
Additional tests may include:
Retinal photography
Optical Coherence Tomography (OCT)
Retinal angiography (if required)
Early diagnosis helps prevent permanent damage.
» Management & Care (Overview)
The most important step in managing hypertensive retinopathy is strict control of blood pressure.
General management includes:
Controlling blood pressure with lifestyle changes
Taking prescribed BP medications regularly
Treating associated conditions like diabetes and cholesterol
Regular eye monitoring
Advanced cases may require specialised retinal care, depending on severity.
» Precautions to Protect Your Vision
Monitor blood pressure regularly
Reduce salt intake
Eat a balanced, heart-healthy diet
Exercise regularly
Avoid smoking and excessive alcohol
Manage diabetes and cholesterol
Get regular eye check-ups even if vision is normal
High blood pressure is often called the “silent killer” because symptoms may not appear until damage has occurred.
» When Should You See an Eye Doctor?
Consult an eye specialist if:
You have high blood pressure (even without symptoms)
Vision becomes blurred or distorted
You notice sudden vision changes
You experience frequent headaches with visual issues
Annual eye screening is strongly recommended for patients with hypertension.
1. Mild to Moderate Non-Proliferative Diabetic Retinopathy (NPDR)
Small retinal blood vessel leaks
Mild retinal swelling
Often asymptomatic
2. Severe Non-Proliferative Diabetic Retinopathy
Blocked blood vessels
Reduced oxygen supply to retina
Higher risk of progression
3. Proliferative Diabetic Retinopathy (PDR)
Growth of abnormal new blood vessels
Risk of retinal bleeding
Can lead to retinal detachment and severe vision loss
Diabetic Macular Edema (DME)
Diabetic macular edema occurs when fluid accumulates in the macula, the central part of the retina responsible for sharp vision.
Can occur at any stage of diabetic retinopathy
Major cause of vision impairment in diabetics
Affects reading, driving, and facial recognition
Who Should Get Screened?
Regular eye screening is essential for:
All diabetic patients (even with good vision)
Newly diagnosed diabetics
Pregnant women with diabetes
Patients with long-standing or poorly controlled diabetes
🕒 Annual retinal examinations are strongly recommended.
Can Diabetic Retinopathy Be Prevented?
While it cannot always be avoided, progression can be significantly reduced by:
Strict blood sugar control
Managing blood pressure and cholesterol
Regular eye examinations
Healthy lifestyle and diet
Avoiding smoking
Early detection allows timely planning before vision loss occurs.
When Should You See an Eye Specialist?
Immediately after diabetes diagnosis
If vision becomes blurred or distorted
If floaters or dark spots appear
If sudden vision loss occurs
Prompt evaluation can save vision.
OUR SERVICES
Hypertensive Retinopathy FAQs
In the early stages, controlling blood pressure can help improve symptoms, but once significant damage has occurred, it may not be fully reversible.
The most effective treatment is managing and controlling high blood pressure through lifestyle changes and medications.
High blood pressure damages the blood vessels in the retina, leading to swelling, bleeding, and, in severe cases, retinal detachment or optic nerve damage, which can cause vision loss.
Yes, in severe cases, untreated hypertensive retinopathy can lead to permanent vision loss or blindness.
Anyone with high blood pressure is at risk, especially if their blood pressure is not well controlled. People with long-standing hypertension or additional conditions like diabetes or high cholesterol are at higher risk.